Hope and Healing
Dazzling scientific results aren’t, on their own, necessarily meaningful to patients. So, Monica Perez, PT, PhD, vowed to keep working.
By Wynne Parry

When trauma or disease damages the spinal cord—that information superhighway embodied by nerves running through the vertebrae—it disrupts communication between brain and body. In most cases, even when someone loses all control of their limbs, the injury doesn’t completely sever this neurological conduit. Usually, some nerve fibers survive the insult.
For Monica Perez, PT, PhD, these residual connections are a pathway toward recovery.
Perez is currently the scientific chair of the Arms + Hands Lab at the Shirley Ryan AbilityLab in Chicago. She is also a professor of physical medicine and rehabilitation at Northwestern University and a research scientist at the Edward Hines Jr. VA Hospital, both in Illinois.
Fifteen years ago, when she began her first faculty position, Perez set out to activate the residual connections in patients who had lost control of their arms and legs because of injuries to the neck’s cervical spine.
Perez believed that by using electrical and magnetic stimulation, she could strengthen them and, ultimately, help patients regain some of the movements they had lost. In those first experiments, she and Karen Bunday, PhD, a postdoc in her lab, adapted a protocol based on what is known as spike-timing-dependent plasticity, in which researchers use stimulation to tune the strength of neurological connections.
In their first experiment, they focused on the upper body, stimulating activity in the part of the brain that controls the hand by placing a magnetic coil against the patients’ scalps. They then applied an electrical current to the ulnar nerve, which activates muscles in the hand. They went on to stimulate both for a total of 100 times, carefully pairing the timing of the ulnar nerve stimulation with that of the brain’s motor cortex.
“It was just great,” Perez says. “You could see that the size of responses evoked from stimulation of the motor cortex increased or decreased, depending on the timing of the paired pulses, in people who had these injuries for many years.”
What’s more, after the stimulation, the patients could perform a dexterity task of moving small pegs into holes faster than they could before.
From her perspective, the study was a success, but when she spoke with patients afterward, their reactions suggested a more complicated reality. She remembers showing one man in particular the recordings. “It was difficult for him to connect with the results because he just hadn’t seen enough improvement in his ability to use his hand,” she says. “It was a moment when the mismatch between what we’d achieved scientifically and its significance to patients became clear.”
She knew: “To really get to the patient, we need to make this better and stronger.”
A Switch in Careers
A native of Chile, Perez began her career as a physical therapist. Patients with neurological disorders, especially spinal cord injuries, interested her most. She was fascinated by involuntary symptoms such as muscle spasticity and spasms that result from an injury, she says. “I wanted to know ‘how do these symptoms arise?’ And ‘how can we treat them?’”

But over time, she realized that some of the therapies she offered patients lacked a basis in science. And she knew that a better understanding of how the nervous system responds to these injuries could lead to more effective treatments. So, Perez decided to pursue a PhD.
“Even though I loved working as a physical therapist, I decided that I wanted to be on the other side and contribute in a different way,” she says.
She obtained her doctorate at the Miami Project at the University of Miami Miller School of Medicine, where she learned about approaches that can noninvasively activate these connections. Later, at her postdoctoral positions at the University of Copenhagen and the U.S. National Institute for Neurological Disorders and Stroke, she studied electrophysiology and motor control of arm and leg movement.
In the decade since that first study, in which she noticed the disconnect between her promising results and patients’ reactions, she and her group have optimized the protocol considerably. Now, they target multiple muscles in the upper and lower limbs, using stimulation regimens customized to each patient. Patients receive more paired pulses administered in many sessions, which are followed by physical therapy.
Improving Patients' Lives
In a major trial that she and her group recently finished, they tested whether or not stimulation for both the arms and legs, along with exercise, can increase the speed of recovery.
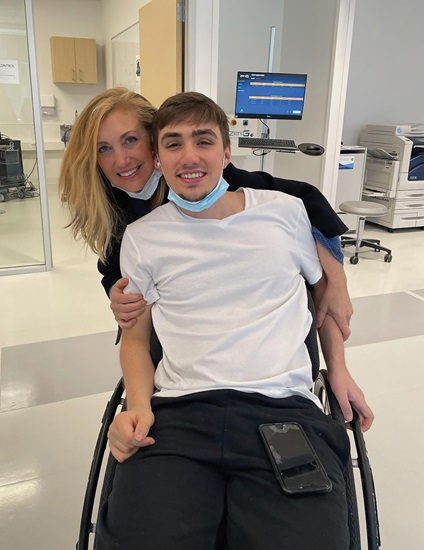
After completing 40 sessions, participant Timothy Brodigan, now 21, has seen clear improvement. In 2017, as a teenager, he suffered a traumatic injury in his neck that impaired his ability to walk and use his arms. Like others in the trial, his injury left him severely weakened but with some voluntary control over his movements.
“I definitely feel stronger. I have regained movements in my legs that I did not have before,” he says. “I have participated in many sessions. After three years of intensive rehabilitation, I hit a plateau. That was very discouraging! The stimulation is definitely helping.”
Roughly a month after starting the trial, Brodigan had improved enough that he felt comfortable walking with a walker with forearm crutches, he says.
Such improvements occur regularly now among patients. “When I discuss the results with them, I don’t need to show them their recordings; they feel stronger and know they have improved in functioning,” Perez says.
She finds the change immensely gratifying: “You feel like you can make an impact, like your scientific efforts are applied and making a difference.”
Family Collaboration
Achieving clear-cut improvements hasn’t dampened Perez’s motivation to understand the mechanisms at work in patients’ nervous systems.

The stimulation could work by increasing communication between neurons and may encourage cells to sprout and connect with other neurons. To better understand these mechanisms—and how to continue to optimize them—she has partnered with her husband, neuroscientist Martin Oudega, PhD, also at the Shirley Ryan AbilityLab, to study this process in a rat model.
The couple met at the Miami Project when Perez was a graduate student. At first, Oudega’s work on cell transplantation in animal models with spinal cord injury appeared to have little in common with Perez’s interest in human physiology. However, they eventually found common cause in studying methods to encourage plasticity in the nervous system, and the two have collaborated heavily for several years.
While they look to explain why the protocol works, Perez faces another question: How far can it go? “We have a couple of individuals who have completed 120 sessions with us, and we haven’t seen their improvement plateau yet. This is very promising,” she says.
Her group is seeking to introduce its stimulation-based approach to other hospitals and to adapt it to help those with complete paralysis. “Right now, the patients with some voluntary control benefit the most, but we want to help everyone with a spinal cord injury,” she says. “And we want everyone to benefit and get better faster and more efficiently.”
This article was originally published in the March 2023 issue of The Physiologist Magazine.
“You feel like you can make an impact, like your scientific efforts are applied and making a difference.”
The Physiologist Magazine
Read the Latest Issue
Don’t miss out on the latest topics in science and research.
Contact Us
For questions, comments or to share your story ideas, email us or call 301.634.7314.


